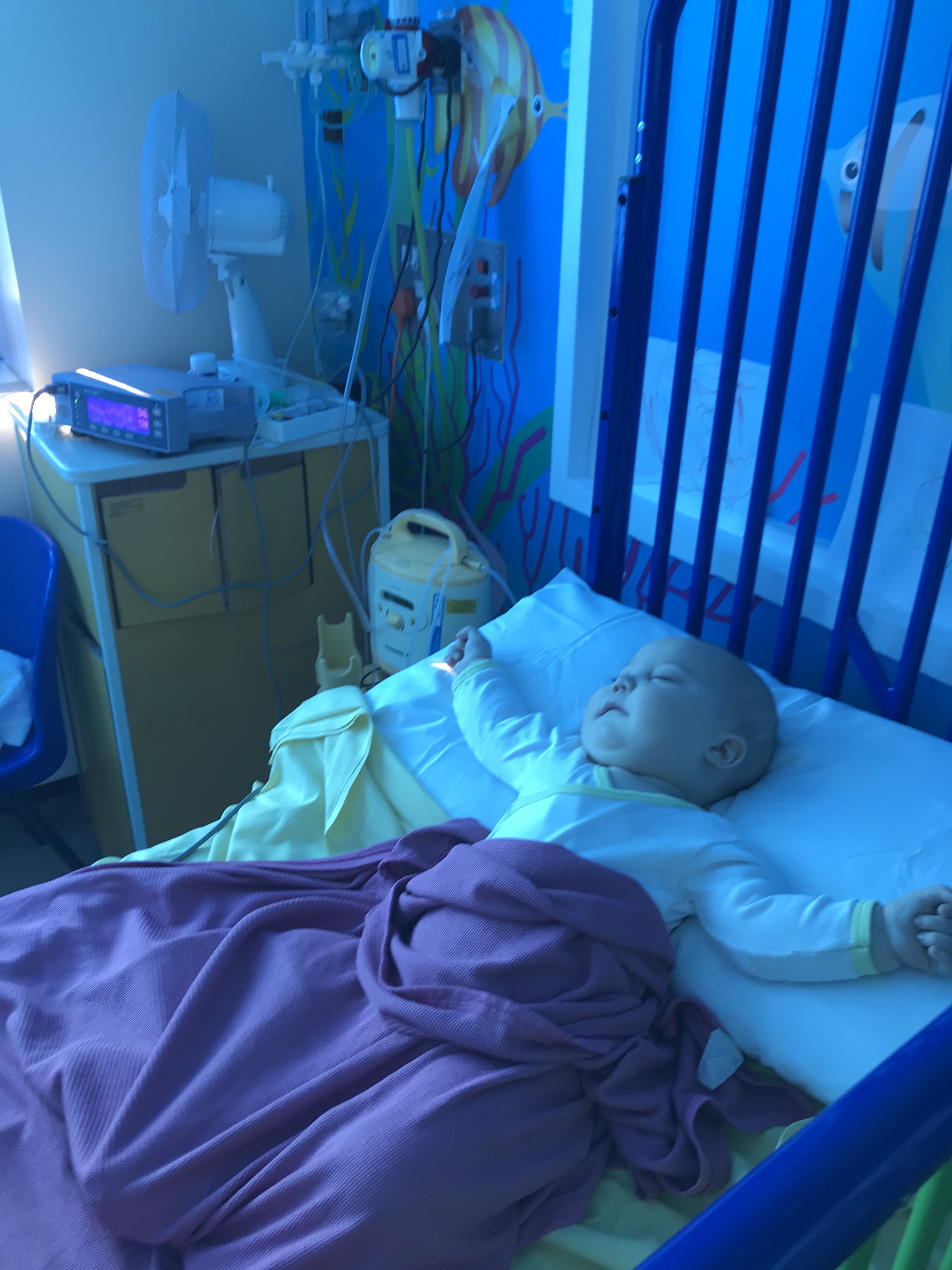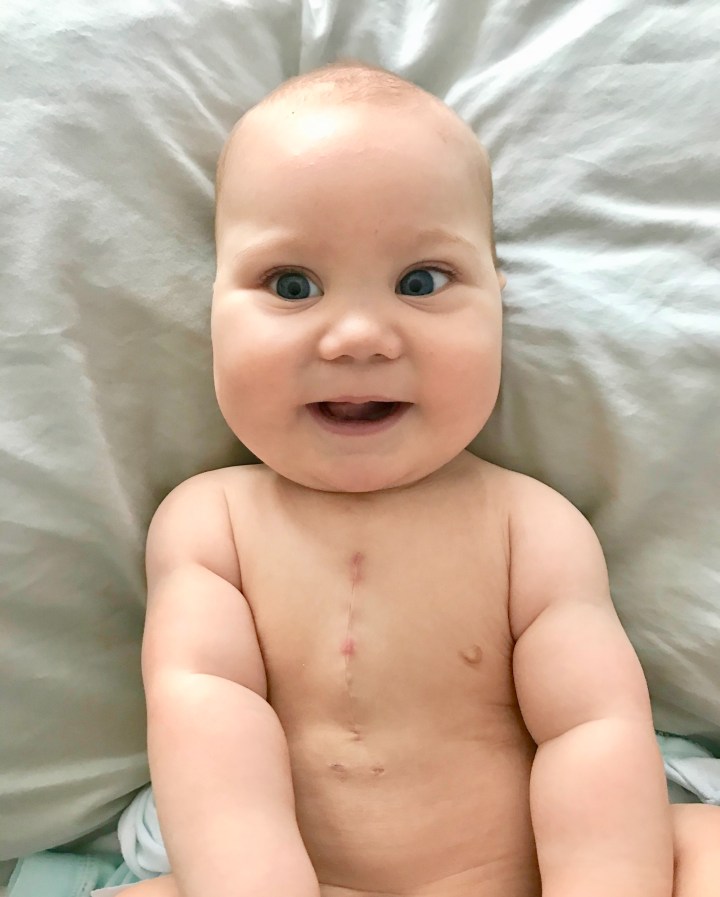
After 16 days in the hospital, Henry and I returned back home. I remained diligent on being involved in the doctor’s rounds each morning which was often attended by a registrar or two (similar to what we would call a resident un the US health system), the head nurse, his assigned nurse and a consultant (doctor) or two. I had heard enough misinformation regarding Henry’s progress in a few of these daily bedside discussions, that I took it upon myself to be ready to take notes and stand up and interject if need be. (I’m sure they LOVED this assertive American 🤭.) If there is one thing I’ve read about managing your healthcare in the UK as opposed to the US, it’s that you have to advocate for yourself. You cannot leave it up to healthcare workers to advocate for you. You have to be comfortable to ask questions and do your own research. Matt and I are so grateful to have family with a healthcare background so we could ask the right questions and know when and what to look out for discrepancies in these meetings. It is not to say these professionals are lacking in their knowledge, and education. The issue we have come across in most instances, is the miscommunication between them regarding the patients status and history. While it was neat to have so many people that were a part of his care team be from so many different countries and backgrounds, the reality is that english is the second language for a lot of them, and on top of that, different dialects can be difficult to understand. It’s easy to see how information can be misconstrued from one shift change to the next. There were enough instances of details missed or wrong that made me think, “what else did they/will they miss?”

After my last update, Henry had blood work done each day to make sure the inflammatory markers were trending back down to normal. They didn’t know what was causing this marker to come back high, but the important thing was that it was trending down. His cardiologist spoke with me and said based on how high a couple of those numbers were, he thought Henry would probably still be there the following week until he fully recovered from whatever was causing that inflammatory marker to spike. He also commented that they would prefer to get him discharged as soon as he’s better, because of all the virus’s, germs, illness etc, that was floating around the hospital that puts a patient at risk. The next morning, Thursday, during the doctors rounds, they said his numbers/markers in the most recent blood test were almost back down to normal. The cardiologist was not present during rounds. I asked the registrar reporting his status update, “Thats great. So lets talk about when he can be discharged.” The registrar leading the rounds said “his cardiologist wants him to stay next week.” Nope. Wrong. Thats not what he said. I told her I believe she misunderstood, and that while he “thought,” Henry would be there the following week still, that did not mean he “wanted,” him to be there. I requested she review that statement with him. The rounds ended, and not more than 15 minutes later, the cardiologist appeared, not knowing the rounds had just come through. I tattled, and told him what the doctor’s said about him wanting to keep Henry another week. He left immediately to go set the plan straight. We were discharged that evening and home by dinnertime with our family. If there has one thing motherhood has given me, it is the confidence to challenge and speak up for what you know is right when it comes to your child, even if it makes you out to be the obnoxious American 🙋🏼♀️.

It has been six weeks since Huck’s Surgery, and four weeks since we returned home. Within days of coming home, Henry picked up bronchiolitis (a respiratory illness related to RSV, that can be very dangerous for a heart kid) from his brother, despite our efforts to keep him in separate rooms at home as much as possible. He had two hospital visits (similar to a clinic visit in the US) to check that his blood oxygen levels were fine, and they were. He was able to recover at home in about eight days without being admitted to the hospital. In that time, he also received a scheduled RSV immunization that he receives routinely every four weeks since he is a CHD- heart kid, to help prevent him from contracting RSV. On Christmas morning, he woke up with bilateral conjunctivitis (pink eye) and a cough progressed throughout the day. When I brought him in to the GP (general practitioner), they listened to his lungs, and his work of breathing had become more labored at that point, so they called an ambulance to come pick us up. This sounds scary if you’re reading this from the US. While his situation was definitely severe, an ambulance ride is more common here than one might think. Since they don’t have the appropriate tools to treat him at the GP, and they want to make sure if he quickly declines on the way to the A&E (ER), the ambulance has the appropriate tools. I had a feeling this may happened, so I packed an overnight bag accordingly.
After one night of assisted oxygen, two days of nasal-gastric tube feeding, Henry was able to feed orally without getting too fatigued and we were released home on day three. The first two nights in the hospital, he would only sleep for ten to twenty minutes at a time, it was absolute hell. After enduring it the first night, I tapped out and Matt came in to take the second shift. I was able to go home and spend some much needed quality time with Dexter and Shepard, and get an uninterrupted nine glorious hours of sleep. As stressful and scary as this all is, we also have two older children at home that we are mindful of making sure there lives don’t get too interrupted by what Henry is going through. They are such great kids, and adore him so much. Even 2 yo Shep will sometimes say, “Mom, I think Henry’s getting better, he doesn’t go to hospital.”

Henry is still recovering with a slight cough at home, but is back to himself more each day smiling and playing. While this doesn’t affect his heart, it has hindered us from seeing how his day to day quality of life will be with the new anatomy of his heart in between surgeries. We have a three-to-six- month time frame for his next surgery and that depends on how he will get on with the dynamics of how his heart is functioning with the repairs they made and what remains. He is still hitting emotional and cognitive milestones, but his gross motor skills have been set back a bit from spending so much time inclined on a hospital bed. He has lost a significant amount of weight, dropping down to the 37 percentile, when he was consistently at the 75 percentile since he was born. The weight loss is due to him being sick and not feeding efficiently, while the medications he’s on (two diuretics daily) also flush a lot out of his system. Coughing fits while he was sick made it hard to keep much down after feeds as he would cough so hard, then vomit. The good news is that his smile is back and brighter every day, and the fog is lifting while we wait to hear more on his next surgery date.